On an annual basis, ACHC reviews the standards for each accreditation program to ensure relevancy. Generally the revisions are minor and include additions, deletions, and clarifications. The 2019 revisions were released February 1. All deletions and clarifications became effective February 1. New standards and additions to standards become effective June 1.
Annual ACHC Standard Updates
Feb 27, 2019 2:11:32 PM / by ACHC posted in ACHC Today, DMEPOS, Home Health, Hospice, PCAB, Private Duty, Programs, Rx, Sleep
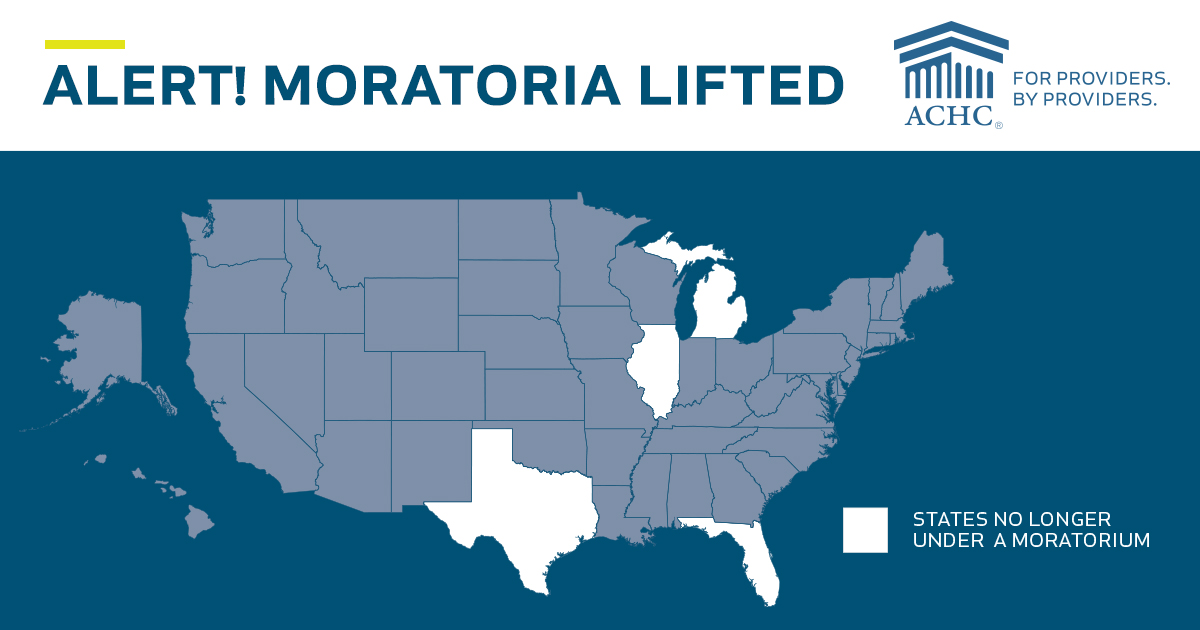
CMS Lifts Home Health Moratoria in FL, TX, MI & IL
Jan 31, 2019 2:43:59 PM / by ACHC posted in Accreditation, ACHC Today, CMS, Florida, Home Health, Illinois, Medicare, Michigan, Moratoria, Programs, texas, Uncategorized
According to the Centers for Medicare & Medicaid Services (CMS), “As of January 30, 2019, there are no active Medicare Provider Enrollment Moratoria in any State or U.S. territories.” CMS announced Wednesday that the provider enrollment moratoria on home health agencies in Illinois, Michigan, Texas, and Florida have expired. The notice from CMS can be read here.
Mapping Community Palliative Care
Aug 14, 2018 2:15:31 PM / by ACHC posted in ACHC Today, Hospice
Palliative care is well established in U.S hospitals, with seventy-five percent of those with fifty beds or more reporting a palliative care program. Recognizing the needs of seriously ill patients and their families in all care settings, many palliative care programs are working to extend services in their communities – either by expanding existing hospital programs to other settings, or building new programs in non-hospital settings. These programs provide palliative care in patient’s homes, nursing homes, doctor’s offices, and outpatient clinics, and are vital in reaching a patient population that would otherwise not be served through traditional hospital palliative care. However, little is known about the locations or extent of this community reach, or how these community palliative care services are staffed and structured to meet patient and family need.
Key Steps to Opening a Medicare-Certified Home Health Agency
Mar 23, 2018 9:38:04 AM / by ACHC posted in ACHC Today, Home Health
While starting a new skilled home health agency (HHA) can be exciting and rewarding, it can also be a long and time-intensive process. Although there is a growing need for HHAs with the population of people age 65 and older expected to reach 19.6 percent by 2030, CMS in recent years has imposed significant financial and operational barriers that HHAs must navigate.
ACHC Approved for Ongoing Home Health and Hospice Licensure Surveys by State of Maryland
Jan 19, 2018 11:01:36 AM / by ACHC posted in ACHC Today, Home Health, Uncategorized
In a recent press release, Accreditation Commission for Health Care (ACHC) announced its approval by the Maryland Department of Health, to perform accreditation surveys in lieu of ongoing state licensure surveys for Home Health agencies and Hospices, in accordance with state law.
ACHC Accreditation – A New Option for California Home Health Licensure
Jan 3, 2018 9:04:57 AM / by ACHC posted in ACHC Today, California, Home Health, home health care news, Licensure, Uncategorized
With more than 500 initial licensure applications pending approval in California, home health agencies are being forced to wait up to two years before receiving their license. To help combat this delay, the California Department of Public Health (CDPH) has given home health agencies the option of working with a CMS-deemed accreditation organization to obtain an initial licensure survey. CDPH is encouraging home health agencies to take advantage of this new option in order to expedite their licensure approval process.
The Changing Healthcare Environment: An Interview with Kim Bradley, Nurse Executive of Sentara Enterprises
Dec 14, 2017 11:23:21 AM / by ACHC posted in ACHC Today, Home Health, Uncategorized
On Behalf of ACHC, the Remington Report interviewed Kim Bradley, Sentara Enterprises, to get insights into the changing healthcare environment and how her organization is handling the challenges. For more than a decade, Sentara has been ranked as one of the nation's top integrated healthcare systems. Their not-for-profit system includes advanced imaging centers, nursing and assisted-living centers, outpatient campuses, physical therapy and rehabilitation services, home health and hospice agency, a 3,800-provider medical staff and four medical groups.
National Home Care & Hospice Month - Stories from Hospice in the Pines' We Honor Veterans Program
Nov 30, 2017 3:09:54 PM / by ACHC posted in ACHC Today, Home Health, Hospice, Uncategorized
November is National Home Care & Hospice Month, and the National Hospice and Palliative Care Organization’s (NHPCO) theme for this year is “It’s about how you live!”
National Home Care & Hospice Month - Share Your Story with ACHC!
Nov 17, 2017 10:00:54 AM / by ACHC posted in ACHC Today, Home Health, Hospice
November is National Home Care & Hospice Month, and the National Hospice and Palliative Care Organization's (NHPCO) theme for this year is "It's about how you live!"
Now Available: ACHC Home Health Standards & Educational Resources - Revised Medicare CoPs
Nov 15, 2017 9:30:19 AM / by ACHC posted in ACHC Today, Home Health, Uncategorized
On January, 9, 2017, CMS finalized the first major revision to the Medicare Home Health Conditions of Participation (CoPs) in more than 20 years. The implementation date for these new CoPs is January 13, 2018 and the phase-in date for Performance Improvement Projects is July 13, 2018, with all other QAPI requirements effective January 13, 2018.